Simulation has emerged as the backbone of “med-ed,” but technology alone isn’t a guarantee of success. If a space doesn’t feel clinical, students won’t feel like healthcare providers. To fully inhabit the role, the classroom must disappear.
Forward-thinking colleges and universities are leveraging seven interior design strategies to boost engagement and send aspiring professionals into clinical environments with confidence.
1. Materials that Withstand Wear & Care.
Finishes set the baseline for student experience. Porous materials, including some plastic laminates, are known to trap contaminants. Nonporous materials resist staining and microbial buildup. These surfaces — such as welded seam vinyl flooring and solid surface counters — withstand rigorous cleaning protocols.
Advanced simulation laboratories, where training may include fluids, reinforce hygiene and infection control, preparing students for patient rooms where spills and sanitization are routine.
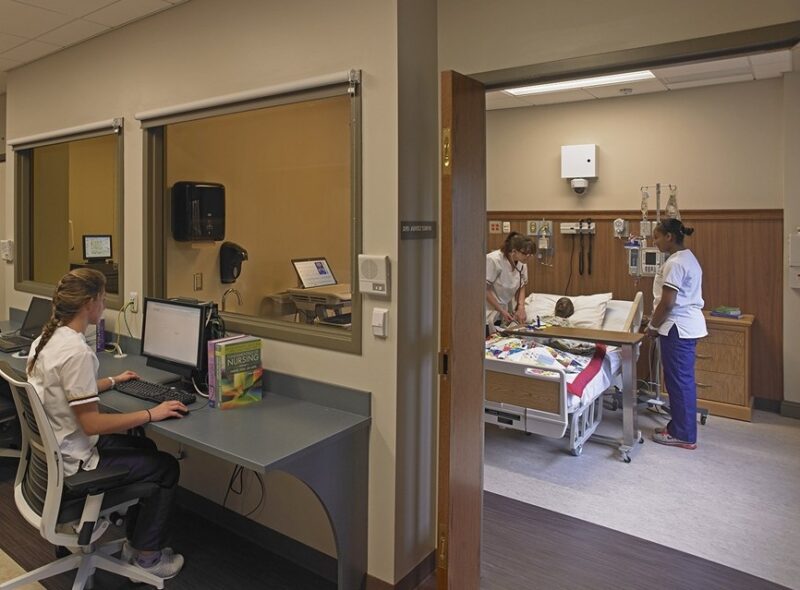
Nazareth University’s School of Nursing features lifelike adult and child manikins that speak, breathe, and blink, cultivating a truly hands-on experience.
2. Layouts that Adapt to Learning.
Healthcare is always changing, and classrooms should too. Multipurpose rooms with modular furniture and teaching zones allow programs to pivot quickly from small group to full-team work — keeping curricula responsive to new modalities, accreditation requirements, and enrollment rates without additional capital investment.

At Roberts Wesleyan University’s Crothers Science and Nursing Center, labs are paired with adjacent informal seating areas that give students space to step out, regroup, and collaborate in smaller teams. This seamless flow between instruction and breakout discussion empowers multiple learning modes without interrupting the lab environment.
Equally important is the infrastructure behind the floors, walls and ceilings: raised platforms, overhead cable trays, and accessible power/data can accommodate a wide range of classes and AR/VR tools, avoiding major renovations when adding or relocating programs.
And as hospitals shift toward decentralized care stations, simulation labs are following suit. Replacing traditional nurse’s stations with several smaller satellite touch-down spaces better reflects today’s mobile reality, giving learners an authentic training experience.
3. Nature Integration for Focus & Recovery.
A simulation environment requires students to quickly move between focused concentration and high mobility tasks. Biophilic elements that connect us with nature ease that experience by providing elements proven to decrease stress. Plants, large windows, organic textures, and soft, natural palettes — such as wall and ceiling treatments depicting the outdoors, daylight, or a blue sky — have a measurable grounding effect on people.
Where windows aren’t feasible, graphic landscaped wall coverings, nature‑inspired artwork, and subtle LED lighting can provide similar relief. Research shows that even brief exposure to daylight is significant: in one study, 97% of students reported greater refocus when given just 5–10-minute views of outdoor scenery, live or artificial.
Additional reports link biophilia to lowering blood pressure, levels of anxiety or anger, as well as increasing levels of attention and memory retention. These all translate into steadier decision-making and learner readiness.
4. Circulation that Mirrors Clinical Workflows.
How people maneuver through a space directly influences how they’ll perform within it. Circulation patterns that replicate the movement on hospital floors — linking patient and control rooms, supply areas, and debrief spaces — help students understand spatial navigation and prioritize high pressured tasks.
Back-of-house routes matter too. Faculty and technicians need discreet pathways, including observation rooms with one-way glass, to monitor performance and re-stage scenarios while safeguarding simulation continuity.

Mindful adjacencies can also enhance interdisciplinary learning — at St. John Fisher University, connecting the nursing and pharmacy programs allowed students to reenact a full medication-management sequence spanning prescription, verification, and delivery.
5. Lighting that Sets the Scene.
Lighting immediately conveys how a space is meant to be used. Adjustable ambient lighting enables instructors to transition seamlessly from bright, even illumination for general assessment, to the low light needed for specialties like ophthalmology.
Additionally, providing the same light fixture types and color temperatures that are used in medical spaces help students acclimate to sensory changes before entering clinical rotations. Because simulations can run for hours, glare control (recessed lights, louvers, and diffusers) remains essential to minimize eye strain.
6. Soundscapes that Build Situational Awareness.
Incorporating realistic auditory signals in healthcare education environments (monitor alarms, pagers, hallway chatter, overlapping conversations) trains students to filter and “triage” mission-critical information in distraction-rich settings.
Attention to acoustic design ensures active simulation spaces do not negatively impact adjacent learning spaces. Through thoughtful implementation of absorptive materials, baffles, and sound panels, noise stays where it belongs — inside the lab — preserving quiet for nearby classrooms and study lounges.
7. Indoor Air that Enhances Performance.
Reliable ventilation, air filtration, and thermal control promote physical wellness and support the safe use of cleaning agents. Coordinating mechanical systems with interior design is critical to meet air quality requirements in a timely, cost-efficient manner. Careful placement of air handling units, ductwork, and compressors helps to maintain acoustic performance, avoids conflicts with nearby spaces, and reduces future maintenance re-work.
Designing What’s Next
Future-ready healthcare education depends on anticipating change, not reacting to it. When workflows, technology, and institutional goals are aligned, health science departments gain the flexibility to evolve and meet rising accreditation demands and clarity about enrollment scale without disruption.
Beyond an aesthetic solution, the result is a deeply immersive program where students hone the skills and intuition needed to excel starting on the first day on the job.


